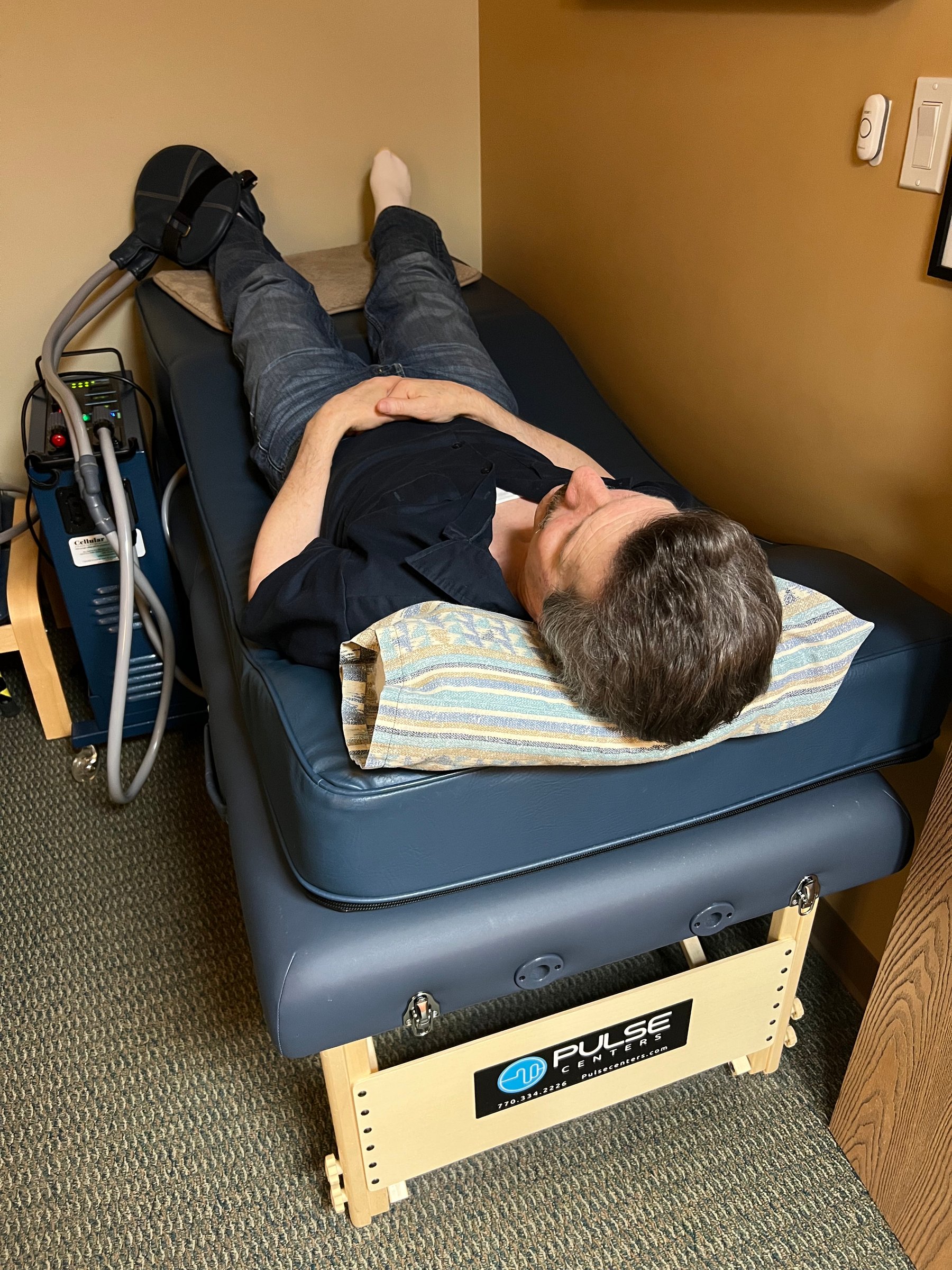
Pulsed electromagnetic fields (PEMFs) have been used in almost every conceivable human illness or malady, including many inflammatory diseases such as arthritis or psoriasis.
PEMF therapy has been associated with pain reduction, and accelerated healing. PEMFs exert these effects by regulating processes involving inflammation and autoimmune diseases, among other biologic actions.
WHAT IS INFLAMMATION?
Inflammation is a cascade of physiological processes instigated by the body to repair cellular damage in tissues with good blood supply and to restore the tissue to its normal function.
Characteristic signs and symptoms that accompany inflammation include: – redness generated by increased blood flow, – heat generated by the metabolism of immune system cells, including leukocytes and macrophages recruited to the damaged site, – swelling due to edema, and – pain caused by the production of pro-inflammatory chemicals named prostaglandins.
Inflammation is the net result of a cascade of biologic processes that is generated and supported by the interaction of a number of immune cell types, including lymphocytes, macrophages and neutrophils, with other cell types such as the fibroblasts, endothelial cells and vascular smooth muscle cells playing a regulatory role in the cascade.
Basically, inflammation is your body trying to heal itself from an injury or other disruption.
ACUTE VS. CHRONIC INFLAMMATION AND INJURY RECOVERY
While inflammation is a necessary and beneficial process, its intensity during the initial acute phase can be abnormally exaggerated, and often persists longer than necessary, developing into chronic inflammation.
Chronic inflammation is associated with dysfunction of one or more parts of the immune system and leads to the ongoing tissue damage found in diseases like tendinitis, arthritis or psoriasis. Chronic inflammation is also a cause of cancer and Alzheimer’s disease, among many other disease conditions.
WHAT CAUSES INFLAMMATION IN THE BODY?
The various cell types and metabolic pathways that generate inflammation provide numerous targets for therapies aimed at controlling inflammation in the acute phase and in preventing progression to chronic inflammation. Inflammation can be initiated by many causes, and knowing and understanding the nature of the cause is important in designing therapeutic approaches.
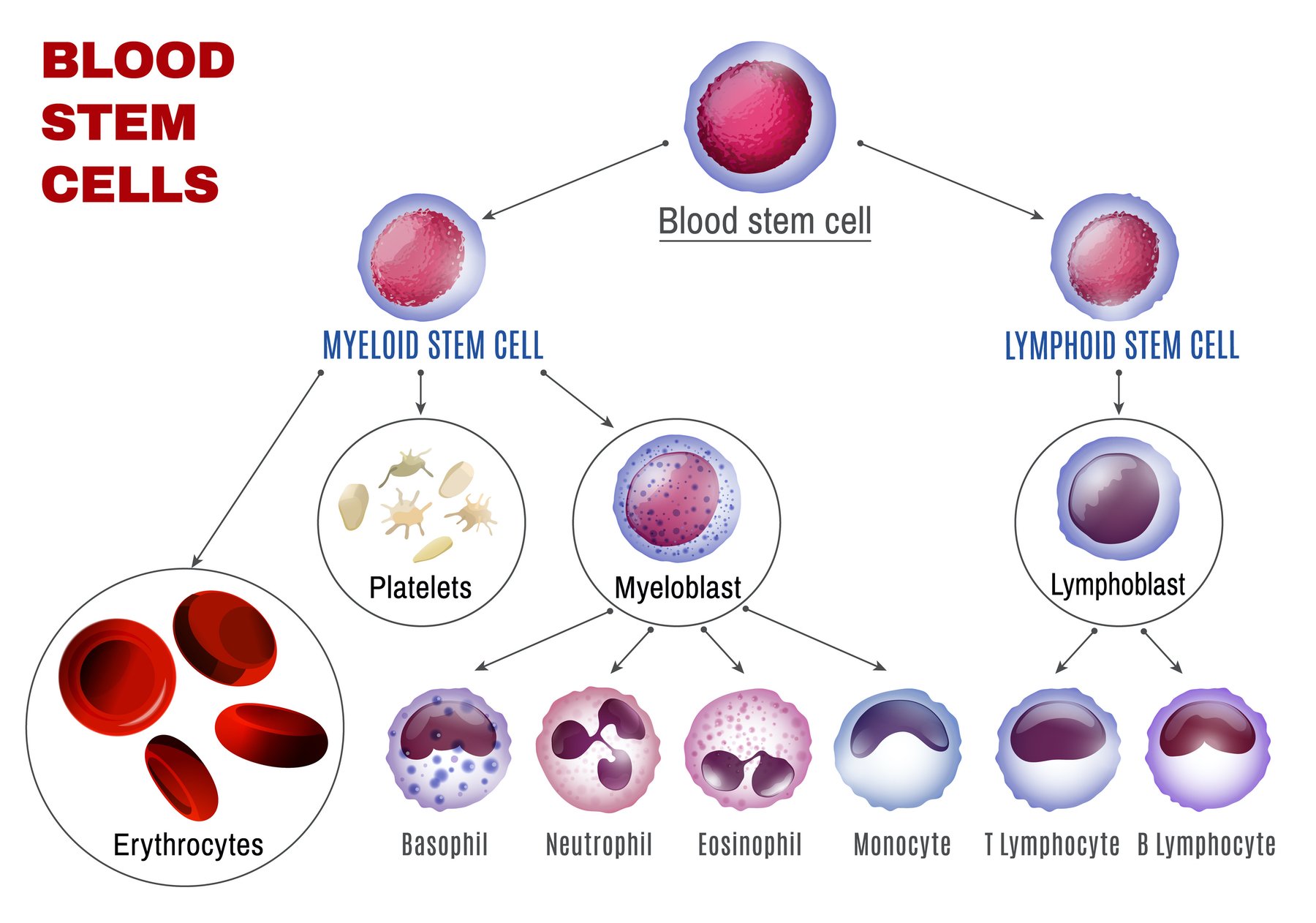 In bacterial infections, early infiltration of the affected tissues by polymorphonuclear neutrophils (PMNs), a type of white blood cell, is followed by the arrival of T cells, an event that is required to kill bacteria. In this circumstance, eliminating T cells can delay or stop healing. In trauma-induced injury, T cells are less important for healing tissue damage, and may be harmful if present for long periods. In this case early elimination of T cells in the acute phase of inflammation could minimize the unwanted effects of inflammation, accelerate healing, and reduce the risk of chronic inflammatory disease. In chronic inflammatory diseases such as rheumatoid arthritis, psoriasis, and chronic tendinitis, persistence of the disease state depends on the presence of T cells. Here, removing T cells would be a favorable approach of therapy for these and similar chronic conditions.
In bacterial infections, early infiltration of the affected tissues by polymorphonuclear neutrophils (PMNs), a type of white blood cell, is followed by the arrival of T cells, an event that is required to kill bacteria. In this circumstance, eliminating T cells can delay or stop healing. In trauma-induced injury, T cells are less important for healing tissue damage, and may be harmful if present for long periods. In this case early elimination of T cells in the acute phase of inflammation could minimize the unwanted effects of inflammation, accelerate healing, and reduce the risk of chronic inflammatory disease. In chronic inflammatory diseases such as rheumatoid arthritis, psoriasis, and chronic tendinitis, persistence of the disease state depends on the presence of T cells. Here, removing T cells would be a favorable approach of therapy for these and similar chronic conditions.
HOMEOSTASIS AND CELLS OUT OF BALANCE
T cells are a major regulator of the inflammatory cascade. Research has shown that PEMFs can induce the appropriate death of T lymphocytes, by actions on T cell membranes and key enzymes in cells. For example, PEMFs have been found to affect ion flow through specific cell membrane channels, including those for sodium, potassium and calcium, that positively affect these enzymes. These appropriate effects help with reducing chronic inflammation.
PEMF-induced changes in ion flow have been associated with the regulation of enzymes involved in inflammation pathways. For instance, PEMFs have been reported to decrease the activity of enzymes associated with the production of inflammatory mediators, such as cyclooxygenase-2 (COX-2) and inducible nitric oxide synthase (iNOS). These enzymes play crucial roles in the inflammatory response, and their downregulation can contribute to the reduction of chronic inflammation.
While the exact mechanisms through which PEMFs affect ion channels and subsequent enzyme activity are still being investigated, the potential therapeutic implications are promising. By modulating ion flow and enzyme activity, PEMFs may offer a non-invasive approach to mitigate chronic inflammation, which is a common factor in various health conditions.1,2
Normal cells are not usually impacted by magnetic fields. Compromised cells, called meta-stable cells, are more likely to be impacted. This means that PEMFs have more impact in circumstances where there is imbalance in tissues or cells, i.e. where there is pathology or chronic inflammation. Where homeostasis in the body is robust, PEMFs, especially weaker PEMFs, are unlikely to have effects. For example, activation of the T cell receptor, such as happens with PEMFs, also activates various processes in the cell that within five minutes after removing the activating signal, these activated processes return to normal levels.
REDUCTION OF INFLAMMATION AND PAIN WITH PEMFS
Significant changes occur in other white blood cells called lymphocytes, from both low intensity, low-frequency PEMFs and even DC/permanent magnetic fields. PEMFs interact with cellular systems in often unexpected ways. This means that increasing frequency and or intensity does not always produce a one-to-one change in reaction intensity.
PEMFs inhibit growth and the natural death of unwanted lymphocytes that decreases inflammation. The PEMF inhibition of lymphocytes and then inflammatory processes appears to be most obvious 48 and 72 hours after PEMF treatment and then the PEMF effect seems to disappear. This indicates that the effects of PEMFs can work well with other natural treatments.
USING PEMF THERAPY FOR TENDONITIS, ARTHRITIS AND SIMILAR CONDITIONS
PEMF use for inflammation needs to be optimized so that exposure will lead to long-lasting, therapeutically relevant outcomes. Pulse-burst-modulated higher frequency fields seem to be much more effective than other frequency signals, and therefore produce improved therapeutic outcomes. While particular types of signals may be most effective, a positive response is often seen to various kinds of magnetic stimuli. There appear to be similar effects on lymphocytes using pulsed bone healing fields, versus sinusoidal power line frequency fields.
Pulsed PEMFs with intensities from 5-25 MilliTesla had no effects on normal T cells. This means there is no apparent damage to normal lymphocytes. Inflammatory T cells produce interleukin-2 (IL-2), which stimulates growth of T cells. When IL-2 levels are high enough, it increases desired early elimination of these chronic inflammatory cells. Cells exposed to pulsed PEMFs can make up to a threefold increase in IL-2.3
There appear to be PEMF intensity windows, but these have not been well defined. Frequency windows have been found to vary across different types of tissue cells in the body. The frequency ranges appear to be quite narrow for bone cells. For lymphocytes the frequency windows seem to be broader. Even 5-100 hertz, 0.15 mT signals modulate calcium flux in lymphocytes, 50 Hz PEMFs having the greatest effect. Frequency fields, combined with parallel static magnetic fields have also been found to have action.
It is important to know that PEMFs affect all lymphocytes, including B cells and T cells and other human lymphoid cell lines.4
HOW PEMFS CAN HELP INFLAMMATION AND PAIN
PEMF therapy specifically targets cells that are meta-stable as a consequence of disease or other ongoing therapies. Thus, PEMFs can be an important cellular therapy in many diseases, including cancer, psoriasis, wound healing, and bacterial infections because of their effects on reducing chronic inflammation. It is important that normal homeostatically stable cells are not harmed by PEMFs, allowing other treatments to be more effective without proportional increases in side effects.5
In chronic inflammatory diseases, cells are characteristically maintained in meta-stable states, as a consequence of cytokine secretions and other stressors associated with the disease. In these cases, PEMFs can work as a stand-alone anti-inflammatory therapy. Even weak, low-frequency PEMFs induce apoptosis in activated T cells, thereby reducing chronic inflammation without negatively affecting acute inflammation.
Overall, PEMF is an ideal therapy for both acute and chronic inflammation and pain conditions due to the way that it interacts with our biology on a cellular level. By correcting physiological imbalances pain is reduced in the short term while long term healing and recovery is optimized.
If you want to find out more, check out what makes my philosophy unique among health care providers.
Always remember one of my mantras, "The more you know about how your body works, the better you can take care of yourself."
For more details about the natural approach I take with my patients, take a look at the book I wrote entitled: Reclaim Your Life; Your Guide To Revealing Your Body's Life-Changing Secrets For Renewed Health. It is available in my office or at Amazon and many other book outlets. If you found value in this article, please use the social sharing icons at the top of this post and please share with those you know who are still suffering with chronic health challenges, despite receiving medical management. Help me reach more people so they may regain their zest for living! Thank you!
ALL THE BEST – DR. KARL R.O.S. JOHNSON, DC – DIGGING DEEPER TO FIND SOLUTIONS
References:
1. Cadossi R, Massari L, Racine-Avila J, Aaron RK. Pulsed Electromagnetic Field Stimulation of Bone Healing and Joint Preservation: Cellular Mechanisms of Skeletal Response. J Am Acad Orthop Surg Glob Res Rev. 2020 May;4(5):e1900155. doi: 10.5435/JAAOSGlobal-D-19-00155. PMID: 33970582; PMCID: PMC7434032.
2. Flatscher J, Pavez Loriè E, Mittermayr R, Meznik P, Slezak P, Redl H, Slezak C. Pulsed Electromagnetic Fields (PEMF)-Physiological Response and Its Potential in Trauma Treatment. Int J Mol Sci. 2023 Jul 8;24(14):11239. doi: 10.3390/ijms241411239. PMID: 37510998; PMCID: PMC10379303.3. Hua, H., Yang, W., Zeng, Q., Chen, W., Zhu, Y., Liu, W., Wang, S., Wang, B., Shao, Z., & Zhang, Y. (2020). Promising application of Pulsed Electromagnetic Fields (PEMFs) in musculoskeletal disorders. Biomedicine & Pharmacotherapy, 131, 110767. https://doi.org/10.1016/j.biopha.2020.110767
4. Luo, Fei & Hou, Tianyong & Zhang, Zehua & Xie, Zhao & Wu, Xuehui & Xu, Jianzhong. (2012). Effects of Pulsed Electromagnetic Field Frequencies on the Osteogenic Differentiation of Human Mesenchymal Stem Cells. Orthopedics. 35. e526-31. 10.3928/01477447-20120327-11.
5. Hollenberg AM, Huber A, Smith CO, Eliseev RA. Electromagnetic stimulation increases mitochondrial function in osteogenic cells and promotes bone fracture repair. Sci Rep. 2021 Sep 27;11(1):19114. doi: 10.1038/s41598-021-98625-1. PMID: 34580378; PMCID: PMC8476611.